Introduction
Depression and anxiety are the most common mental health conditions worldwide. One out of five adults in the U.S. has one or more forms of mental illness. Food is not only important for keeping the brain fueled and operating but can also protect it from damage and cognitive decline. The food we choose to eat is a powerful way to have some control over our moods and brain function.
Nutrition matters
Nutrition plays a vital role in thinking, behavior, learning, memory and emotions. The components of foods can affect cognition, influence mood and alter physical states. Besides having health effects, there are cultural, social and personal preference factors that affect food choices.
High intake of sodas and snacks, and low fruit and vegetable intake are linked to negative mood. Low micronutrients are also associated with worsening mood.
High intake of saturated fats and refined carbohydrates increases the risk of depression by:
- Promoting inflammation and oxidative stress.
- Disturbing microbiome and gut-brain communication.
- Causing degeneration of the hippocampus (learning/memory).
- Leading to nutrient inadequacies.
Nutrients in foods are precursors to neurotransmitters, chemical messengers which regulate brain function. They regulate heart rate, breathing, sleep, digestion, appetite and mood. They are also closely linked to sight, smell and taste of food.
For example, serotonin, the “feel-good hormone,” is a neurotransmitter made from the essential amino acid tryptophan, which can be found in leafy greens, broccoli, sunflower seeds, mushrooms and soybeans.
Other neurotransmitters include endorphins, dopamine, oxytocin and GABA, all of which are impacted by amino acids found in our food choices.
The role of food
Foods linked with chronic diseases are also linked with depression and other mental disorders. Those with chronic depression and anxiety experience increased heart rate and blood pressure, and increased risk of heart attack and stroke. Dietary recommendations for reducing risk for heart attack and stroke are also beneficial for preventing and managing mental illness and mood disorders.
Those with diabetes are at increased risk for depression, anxiety disorders and eating disorders. The relationship between diet and mental health is complex and may seem unclear. However, diet has been shown to offer a positive path to gaining control over blood sugar, lowering inflammation and reversing insulin resistance. Studies show that diets consistently providing low-glycemic-index foods can reduce depressive symptoms and improve mood.
The glycemic index is a measurement of how much, and how quickly, a food increases blood sugar levels. The lower the glycemic index, the less it may negatively impact blood sugars. High-glycemic foods include sugars, sweetened beverages and refined starchy foods such as bread, pastries and cereals. Lower glycemic carbohydrates include fiber, which helps to control blood sugars. These include fresh fruits and vegetables, 100% whole grains, nuts and seeds.
Those with depression often present with inflammation markers. Diets that promote inflammation are high in saturated fats, trans fats and refined carbohydrates, which have detrimental effects on the brain. These include cognitive decline, damage to the blood-brain barrier, hippocampal dysfunction and increased risk of depression.
Carbohydrates
Depression is associated with consumption of refined carbohydrates, particularly foods with added sugars, foods with a high glycemic index and snack foods. Depressive symptoms are often associated with carbohydrate cravings. Foods with a high glycemic index can help to produce serotonin, which relieves symptoms of negative mood and depression. This effect is only temporary and may result in increasing cravings for poor food choices.
Feeling hangry?
Hangry is the term applied to the state of bad temper or irritability as a result of physical hunger.
Being hangry can cause the release of cortisol and adrenalin associated with stress and tension. Hunger also stimulates the same systems that monitor emotions and hormones. When in this hangry state, we may view neutral events and circumstances in a more negative light.
Comfort foods
Comfort foods are foods associated with good thoughts, good feelings and happy memories. They have been known to evoke a sense of well-being and decrease perception of loneliness. These foods are usually high in sugar or refined carbohydrates, which tend to initiate a high blood sugar response. These are referred to as high-glycemic-index foods.
Serotonin production is driven by insulin release in response to intake of high-glycemic-index foods.
This means that comfort foods work. Foods with a high glycemic index significantly reduce depressive symptoms. So, the question is, do we get depressed when we eat these foods, or do we eat these foods because we are depressed?
The answer is both.
Using foods to feel better may help with negative emotions, but this has only a temporary effect. Our ability to taste sweet is reduced when we are stressed, which can contribute to seeking out more of these foods.
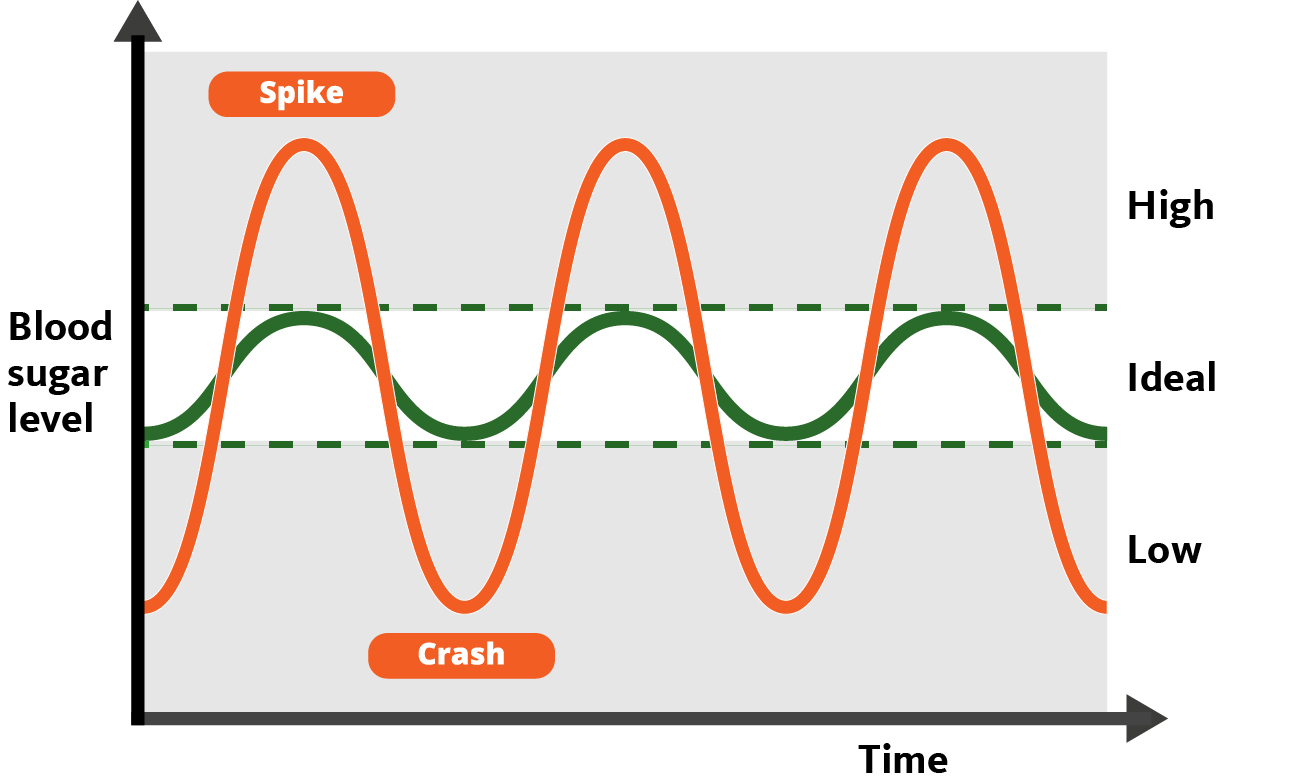
These behaviors contribute to blood sugar spikes and subsequent crashes, which result in irritability, sugar cravings and depression. They can also lead to recurring negative feelings, weight gain and depression associated with low self-control and poor body image.
Recurring hypoglycemia, a state of low blood sugar, is associated with mood disorders. Regulating blood sugar spikes may be the key to stabilizing mood.
Fats
At least 60% of our brain is composed of fat. It plays structural and functional roles and regulates conversion of sensory signals to electrical impulses in the brain.
Essential unsaturated fatty acids are crucial for brain integrity and ability to perform. However, diets high in saturated fat increase the risk of neurological disease. Saturated fats impair brain performance and memory.
Meals high in saturated fat also contribute to inflammation, which is associated with cognitive decline, hippocampal dysfunction and mood disorders. Saturated fat intake is associated with an increased risk of Alzheimer’s disease and other forms of dementia.
Proteins
The brain uses the amino acids tryptophan, tyrosine, histidine and arginine to synthesize neurotransmitters. The foods that contain these amino acids are not created equal.
Animal-based protein foods also contain saturated fat and cholesterol. Plant foods contain all the essential amino acids but do not contain cholesterol, and most plants have little or no saturated fat.
Plant sources of amino acids that contribute to the production of neurotransmitters include:
- Tryptophan: leafy greens, broccoli, sunflower seeds, mushrooms, soybeans
- Tyrosine: legumes, oats, peanuts, pumpkin seeds, spinach
- Histidine: rice, quinoa, cauliflower, buckwheat
- Arginine: soy, walnuts, garlic, sesame, hemp and pumpkin seeds
Micronutrients and phytonutrients
Vitamins, minerals and other plant compounds are required components for neurotransmitter production and mood regulation. Vitamin C is required for making dopamine, noradrenalin and serotonin. Vitamin D regulates serotonin and oxytocin synthesis. Iron helps with recovery from lethargy, and folate improves depressive symptoms.
Nitric oxide, made from nitrates in green, leafy vegetables, or L-arginine in nuts and seeds, is a powerful vasodilator. It helps to lower blood pressure and improve blood flow. It is also important for regulation of norepinephrine, serotonin, glutamate and dopamine.
Gut feelings are not just imagined. They are a series of reflexes between the brain and the gut that affect multiple body systems. Stimuli that induce emotions (fear, anger, love) also induce changes in the gut and brain.
There exists a bidirectional communication between the gut and the brain called the gut-brain axis. This pathway is critical to preventing and treating clinical depression. It affects digestion, gastrointestinal homeostasis, motivation, decision-making, risk of obesity and eating disorders. It is estimated that between 60% and 70% of the body’s serotonin is produced in the gut.
It has been determined that 56% of patients with anxiety and depression have intestinal disturbances related to an imbalance of gut microbes. This imbalance is linked to irritable bowel syndrome, Parkinson’s disease, mood disorders, autism spectrum disorders, depression and Alzheimer’s disease.
Fiber is prebiotic, serving as food for healthy gut microbes. There are two types of fiber: soluble and insoluble. Although healthy gut microbes consume fiber from a variety of plant foods, we should prioritize sources of soluble fiber. These include lentils, beans, oats, barley, flax and chia seeds and the skins of fruits like apples and grapes.
Probiotics are healthy organisms that can populate our gut. We can consume these by choosing fermented foods with live organisms like yogurt, sauerkraut, pickles and kimchi.
Positive mood plant foods
- Unsaturated fats from whole foods, including tree nuts, peanuts, seeds, olives and avocados.
- Complex carbohydrates from intact and 100% whole grains, starchy vegetables like corn and sweet potatoes, leafy greens and cruciferous vegetables.
- Raw, dark green, leafy vegetables and raw beetroots provide compounds for making nitric oxide.
- Plant sources of protein include lentils, beans, split peas and soy products, which are low in fat and cholesterol free.
- Fermented foods with live probiotics.
- Citrus fruits, red peppers, ginger root, green tea, curcumin, lavender and saffron spices.
- Vitamin D from sun exposure, or supplementation, 800 to 2,000 IU/day for adults.
- Sublingual B12 supplements, 50 micrograms per day, 1,000 mc/day if over age 50.
Aromatherapy
- Sense of smell is strongly linked to memories and emotions.
- Food smells and essential oils can relieve anxiety and depression, reduce pain perception and improve sleep.
- Rosemary helps with memory, ginger boosts mood, citrus boosts alertness and lavender eases insomnia and depression.
Best practices
- Avoid processed foods high in salt, sugar, saturated fat and refined carbohydrates (sugars and flours).
- Reduce or eliminate sources of saturated fat, animal meats, cheese and other dairy products.
- Adopt a Mediterranean or plant-based diet high in fruits, vegetables, legumes, nuts and seeds.
- Increase fiber from whole plant foods gradually to 40–60 gm/day to feed healthy gut microbes.
- Add 2–3 tablespoons per day of flax or chia seeds for omega-3 fats.
- Hydrate with water and green tea.
References
Baroni, L., A.R. Sarni and C. Zuliani. 2021. Plant foods rich in antioxidants and human cognition: A systematic review. Antioxidants.
Bavarsad, N.H., S. Bagheri, M. Kourosh-Arami, et al. 2023. Aromatherapy for the brain: Lavender’s healing effect on epilepsy, depression, anxiety, migraine and Alzheimer’s disease: A review article. Heliyon.
Bender A., K.E. Hagan and N. Kingston. 2017. The association of folate and depression: A meta-analysis. Journal of Psychiatric Research. https://www.sciencedirect.com/science/article/abs/pii/S0022395617305927
Bennett, D. 2020. Depression can be identified using gut bacteria, University of Florida Health researchers find. University of Florida Health.
Chianese, R., R. Coccurello, A. Viggiano, et al. 2018. Impact of dietary fats on brain functions. Current Neuropharmacology.
Cornish, S., and L. Mehl-Madrona. 2008. The role of vitamins and minerals in psychiatry. Integrative Medicine Insights.
Dhir, A., and S.K. Kulkarni. 2011. Nitric oxide and major depression. Nitric Oxide.
Dighriri, I.M., A.M. Alsubaie, F.M. Hakami, et al. 2022. Effects of omega-3 polyunsaturated fatty acids on brain functions: A systematic review. Cureus.
D’Onofrio, G., S.M. Nabavi, D. Sancarlo, et al. 2021. Crocus Sativus L (Saffron) in Alzheimer’s Disease treatment: Bioactive effects on cognitive impairment. Current Neuropharmacology.
Firth, J., J.E. Gangsisch, A. Borsini, et al. 2020. Food and mood: How do diet and nutrition affect mental wellbeing? British Medical Journal.
Fung, T.K.H., BW..M. Lau, S.P.C. Ngai, et al. 2021. Therapeutic effect and mechanisms of essential oils in mood disorders: Interaction between the nervous and respiratory systems. International Journal of Molecular Science.
Gangwisch, J.E., L. Hale L., L. Garcia, et al. 2015. High glycemic index diet as a risk factor for depression: Analyses from the Women’s Health Initiative 1. American Journal of Clinical Nutrition.
Heart disease and mental health disorders. Heart Disease, Centers for Disease Control and Prevention.
Huang Q, H. Liu, K. Suzuki, et al. 2019. Linking what we eat to our mood: A review of diet, dietary antioxidants and depression. Antioxidants.
Korn, L.E., 2020. How nitric oxide helps mental health and COVID-19 response. Psychology Today.
Kumar, A., J. Pramanik, N. Goyal, et al. 2023. Gut microbiota in anxiety and depression: Unveiling the relationships and management options. Pharmaceuticals.
Lee, M.F., R. Eather and T. Best. 2021. Plant-based dietary quality and depressive symptoms in Australian vegans and vegetarians: A cross-sectional study. British Medical Journal.
Lieberman, H.R. 1999. Amino acid and protein requirements: Cognitive performance, stress and brain function. National Center for Biotechnology Information, National Library of Medicine, National Institutes of Health.
Liu, L. and G.Zhu. 2018. Gut-brain axis and mood disorder. Frontiers in Psychiatry.
MacFarlane, A.J., Y. Shi and L.S. Green-Finestone. 2014. High-dose compared with low-dose vitamin B12 supplement use is not associated with higher B12 status in children, adolescents and older adults. Journal of Nutrition, Nutritional Epidemiology.
Mitrea, L., S.A. Nemes, K. Szabo, et al. Gut imbalance imbalances the brain: A review of gut microbiota associated with neurologic and psychiatric disorders. Frontiers in Medicine.
Murphy J., 2020. Is being ‘hangry’ a real thing? MDLinx.
Penckofer, S., J. Kouba, M. Byrn, et al. 2010. Vitamin D and depression: Where is all the sunshine? Issues in Mental Health Nursing.
Pullar, J.M., A.C. Carr, S.M. Bozonet and M.C.M. Vissers. 2018. High vitamin C status is associated with elevated mood in male tertiary students. Antioxidants.
Rajan, S., J.I. Wallace, K.I. Brodkin, et al. Response of elevated methylmalonic acid to three dose levels of oral cobalamin in older adults. Journal of the American Geriatric Society.
Ramaholimihaso, T., F. Bouazzaoui and A. Kaladjian. 2020. Curcumin in depression: Potential mechanism of action and current evidence: A narrative review. Frontiers in Psychiatry.
Ruan, Y., J. Tang, X. Guo, et al. 2018. Dietary fat intake and risk of Alzheimer’s disease and dementia: A meta-analysis of cohort studies. Current Alzheimer’s Research.
Sattayahkom, A., S. Wichit, P. Koomhin. 2023. The effects of essential oils on the nervous system: A scoping review. 2023. Molecules.
Seaquist, E.R., J. Anderson, B. Childs, et al. 2013. Hypoglycemia and diabetes: A report of a workgroup of the American Diabetes Association and the Endocrine Society. Diabetes Care.
Swann, O.G., M. Kilpatrick, M. Breslinand W.H. Oddy. 2020. Dietary fiber and its associations with depression and inflammation. Nutrition Reviews.
Understanding diabetes and mental health. American Diabetes Association.
Vitamin D, factsheet for health professionals, Office of Dietary Supplements, National Institutes of Health, U.S. Department of Health and Human Services.
What are neurotransmitters? Queensland Brain Institute.
Wurtman, R.J., J.J. Wurtman. 1995. Brain serotonin, carbohydrate-craving, obesity and depression. Obesity Research.